For many men, achieving a firm, masculine chest is a primary fitness goal. However, when chest tissue persists despite a dedicated gym routine and a healthy diet, it may be due to a condition called gynecomastia. Gynecomastia is the benign (non-cancerous) enlargement of glandular breast tissue in males. It is a common condition that often appears during periods of significant hormonal shifts, such as infancy, puberty, or later in life.
While gynecomastia can cause significant psychological distress or self-consciousness, it is rarely a sign of a serious underlying illness. The condition typically stems from an imbalance between the hormones estrogen and testosterone. When estrogen levels are too high or testosterone levels are too low, the breast tissue can begin to grow.
Understanding the Diagnosis
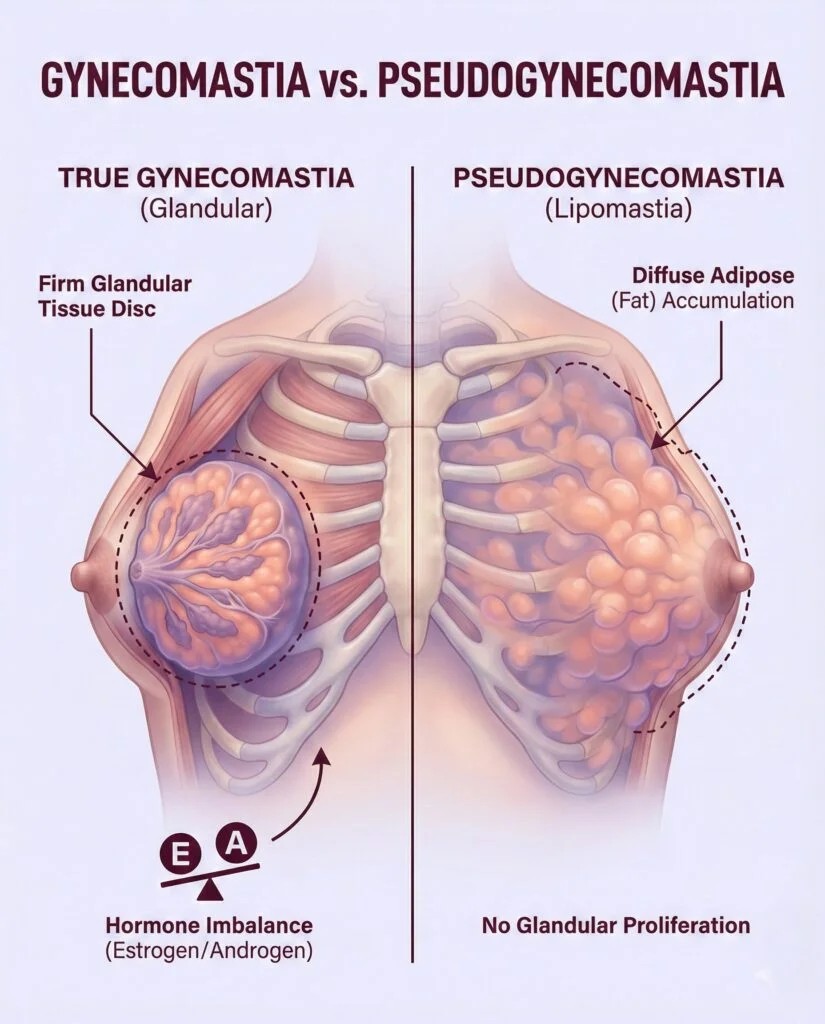
The first step in addressing chest enlargement is determining whether the growth is "true" gynecomastia or "pseudogynecomastia." While they may look similar, their composition is quite different.
- True Gynecomastia: This involves the actual growth of glandular tissue.
- Pseudogynecomastia: This is simply an accumulation of fat in the chest area without any glandular proliferation, often seen in men who are overweight.
To provide an accurate diagnosis, a healthcare professional will conduct a thorough clinical evaluation, which includes two main components:
- Medical History: Your doctor will ask about how long the tissue has been present and if you experience any pain. They will also review your use of medications, herbal supplements, or recreational substances. Certain substances, such as anabolic steroids, spironolactone (a blood pressure medication), and even marijuana, are known triggers for tissue growth.
- Physical Examination: During the exam, a doctor will use "palpation" (feeling the tissue with their fingers). True gynecomastia typically feels like a firm, mobile, disc-like mound of tissue located directly beneath the nipple-areola complex. A testicular exam may also be performed to rule out rare estrogen-secreting tumors.
Diagnostic Imaging and Laboratory Tests
In most cases, a physical exam is enough for a diagnosis. However, if the cause is unclear or if there are suspicious features—such as extreme firmness, nipple discharge, or significant asymmetry—further testing may be required.
- Imaging: A mammogram or ultrasound can help visualize the internal structure of the breast tissue to rule out rare cases of male breast cancer.
- Blood Work: If a natural physiological cause isn't found, doctors may order laboratory tests to check your "hormonal thermostat." These tests often measure levels of testosterone, estradiol, prolactin, and thyroid-stimulating hormone (TSH), as well as markers for liver and kidney function.
Surgical Intervention: When the Gym Isn't Enough
If gynecomastia persists for more than 12 to 18 months, the tissue often undergoes a process called fibrosis. This means the tissue becomes scar-like and permanent, making it highly unlikely to respond to medication or further weight loss. At this stage, surgical intervention is the most effective way to restore a contoured chest appearance.
Liposuction
Liposuction is highly effective for cases where the enlargement is primarily composed of fatty tissue (Grade I and IIa). This procedure involves using a thin tube to suction out excess fat, resulting in a smoother chest contour with minimal scarring.
Subcutaneous Mastectomy
For patients with significant glandular growth, liposuction alone may not be enough. A subcutaneous mastectomy involves the direct surgical excision (removal) of the glandular tissue. This is typically performed through a small "periareolar" incision—a cut made along the edge of the dark skin surrounding the nipple—to ensure the scar is well-hidden.
